Developing a COVID-19 Saliva-Based PCR Testing Method
Story of a Researcher Fighting COVID-19

In an effort to reduce the spread of the COVID-19 pandemic, Professor Takanori Teshima, Director of the Division of Laboratory and Transfusion Medicine at Hokkaido University Hospital, has demonstrated the effectiveness of a saliva-based PCR test method. A reagent kit for detecting novel coronavirus, which was developed by Shimadzu, helped his challenging study in the initial phase.
Shimadzu interviewed Professor Teshima online.
Note: The titles and affiliations of people mentioned in the article were current as of the interview date (August 2020).
Controlling the Spread of COVID-19 Infections
The COVID-19 pandemic arrived in Hokkaido earlier than in any other region in Japan. By mid-April 2020, over 100 active cases were being treated at hospitals in Hokkaido, which could have potentially overwhelmed available healthcare resources.
PCR testing at that time involved healthcare workers acquiring samples by using a cotton swab to wipe mucus from deep inside the nose of patients. In addition to a shortage of staff available for PCR testing and a shortage of masks and protective wear, the swab method carried the risk of infection from patient sneezing or coughing.
Given such a situation, Professor Teshima conducted a study on a scale unprecedented in the world in an effort to establish a saliva-based method of testing for the virus.

Professor Teshima Recalling How “Massive Testing Approach was a Huge Step Forward”
The professor explained that the saliva-based method offers the advantage of being easier and safer to acquire samples than swab sampling and that a person’s mouth provides samples that are always fresh.
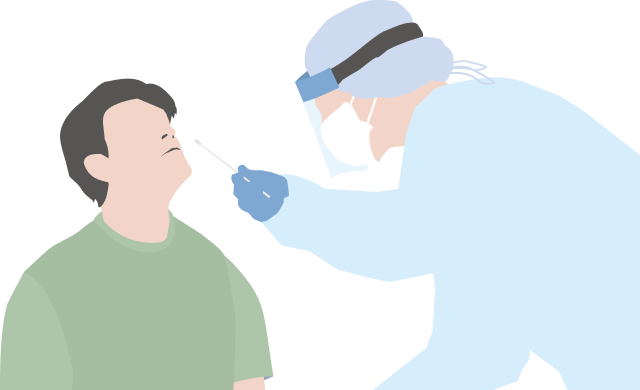
Swab sampling from nasopharynx: Sneezing and coughing may occur during sampling, which causes a risk of infection for healthcare workers. They need to wear protective clothing.

Saliva Sampling: It is safer and easier to obtain samples. Self-collection is also easy.
Fig. Sampling Methods for the Novel Coronavirus Test (created based on interview)
Comment from Professor Takanori Teshima
Regarding COVID-19 infections and testing systems, the professor said, “First of all, keep in mind that everyone can be infected. It could happen to any of us. Therefore, if you test positive, people around you should be allowed to be tested immediately. It is important to establish such a social system.”
He also looks to tech-related companies for further contributions and efforts “to establish reliable technologies and promote innovation in technology.”
Consequently, Shimadzu will keep working hard to utilize our full capabilities to support and respond to the efforts of frontline healthcare workers and researchers to prevent the spread of the pandemic.
 Page Title and URL Copied.
Page Title and URL Copied.


